Pancreatic Cancer Breakthrough
RTÉ Radio 1 DRIVETIME Interview with Prof. Silvia Giordani
 RTÉ Radio 1 • DRIVETIME
RTÉ Radio 1 • DRIVETIMEDrivetime on RTÉ Radio 1 with Sarah McInerney and Cormac Ó hEadhra.
Sarah McInerney: “Patients with pancreatic cancer that is resistant to drugs have been given new hope following a discovery by scientists at Dublin City University. The team at DCU have found a way to successfully treat drug-resistant pancreatic cancer cells in laboratory experiments.”
“Lead researcher Professor Silvia Giordani of the School of Chemical Sciences at DCU is part of the team and she joins us. Now you’re very welcome Silvia to the programme. This week people will have heard that the former England manager Sven-Göran Eriksson was diagnosed with inoperable pancreatic cancer.”
“So perhaps you might explain what the pancreas does and how the pancreatic cancer affects the body.”
Silvia Giordani: “Good evening, Sarah, and thank you very much for having me. Pancreatic cancer is a disease in which malignant cells form in the tissue of the pancreas and they grow out of control, leading to a tumor. And this growth disrupts the pancreas function and can also spread to other parts of the body and what is known as metastasis.”
Sarah McInerney: “So, let me ask you, why is it so severe then and so fatal indeed in many cases?”
Silvia Giordani: “The pancreas cancer is very deadly because of the pancreas location. And it’s located in the middle of the belly tucked behind the stomach and it’s close to vital organs. Some of these cancer cells will travel to other parts of the body via the bloodstream or the lymphatic system - and most often they will also go to the liver, the lungs, the abdominal cavity. It’s an aggressive, rapidly progressing cancer. It grows and it spreads quickly. And treatments are complicated due to the location of the pancreas, which, as I said, is deep in the abdominal location.”
Sarah McInerney: “And of course, another complicating factor is that it’s often not detected early enough.”
Silvia Giordani: “Yes, that’s one of the problems because pancreatic cancer is difficult to detect and diagnose early because of the subtle symptoms. So that, it means that it may go undetected for quite a while until it reaches more advanced stages. The early stage symptoms are vague and so they can be easily mistaken for much less serious conditions.”
Sarah McInerney: “And what are those early symptoms?”
Silvia Giordani: “Common symptoms are pain in the belly, the upper abdomen, and the back, the middle and upper back, and also yellowing of the skin and of the white of the eyes. There could also be an unexpected onset of diabetes, because as we know, pancreas also controls and regulates, by producing insulin controls the level of glucose, and such that if the pancreas doesn’t function, that could lead to diabetes. There could also be severe weight loss, which is common, and digestive issues as well.”
Sarah McInerney: “So how is pancreatic cancer currently typically treated?”
Silvia Giordani: “Surgery can cure pancreatic cancer in its early stage. So the surgeon can remove the affected part of the pancreas. That is, if it didn’t spread to other organs. But surgery may not be possible once the cancer grows large or it extends into the near body blood vessels. In this situation, chemotherapy and radiotherapy are the common treatment.”
Sarah McInerney: “And then can you talk us through, Silvia, what your research and their team’s research have discovered and what difference that might make?”
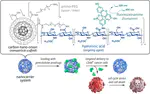
Silvia Giordani: “So in the lab we developed a new drug delivery system to target the cancer cells and to deliver the drugs. In particular, we focused on a very aggressive pancreatic cancer, and so we tested all our delivery system in pancreatic ductal adenocarcinoma cells. And this is because this is a particularly aggressive cancer which is resistant to conventional treatment and has a very high mortality rate. And there is also a lack of effective treatment of effective targeted therapies for this PDAC cancer.”
“What we did was engineering a new transport system for drugs to effectively target the PDAC cells.1 And when we coupled our nano delivery system with therapeutics derived from the traditionally used gemcitabine, which is the anticancer drug, the drug delivery system successfully treated the PDAC cell that have been otherwise resistant.”
“This is of course the result of a collaborative and multidisciplinary research effort like most of the science projects nowadays. And I’d like to mention Michał Bartkowski, which is the PhD student in my team at DCU, funded by the Irish Research Council, and all my collaborators, in particular, Professor Silvia Arpicco and Chiara Riganti, who helped to make this happen.”
Sarah McInerney: “It’s certainly and I always I mean we love covering you know discoveries when it comes to cancer treatment on this program because it’s so good to give people hope and to show what all the research is doing. So what is next then? What will this mean for people and when my people hopefully see some benefit from it?”
Silvia Giordani: “Well, this of course, this is a work done in the cells, in the cancer cell lines, but it does open promising development with targeted therapy. We believe that this is a breakthrough in the sense that we could really show that we were able to target cancer cells that were resistant to the chemotherapy and we could actually show that with this particular drug delivery system, we target them and we can kill them with the drug. So again, this is in cancer cells, which means it will take more research and definitely more effort in order to go towards therapy and treatment.”
Sarah McInerney: “Sure, been a very promising start and thank you very much for joining us to talk us through it. That’s Professor Silvia Giordani from DCU. Thank you.”